Reconstruction Case Studies Beverly Hills
Procedure: Eyelid Rehabilitation
Cosmetic Concern:
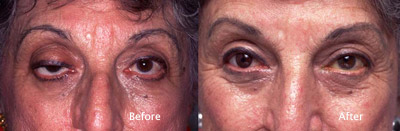
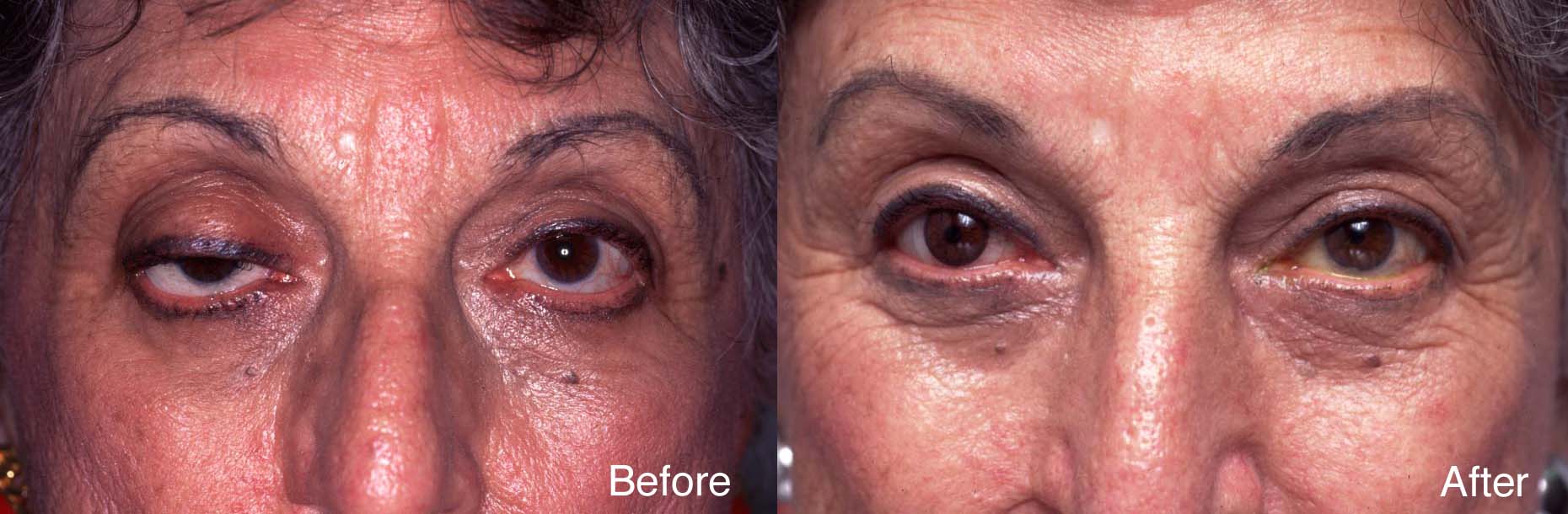
75-year-old woman lost the use of her right eye as a child. She wears a glass shell over the right eye. For the past 50 years, her right upper eyelid has been droopy.
Diagnosis:
- Non-seeing right eye.
- Right upper eyelid ptosis.
Treatment:
- Right upper eyelid ptosis surgery.
- Hand painted contact lens for the right eye.
Discussion:
Once the right upper eyelid ptosis surgery was performed, the ocularist created a hand painted contact lens completing the rehabilitation.
Procedure: Eyelid Cancer Surgery
 Dr. Steinsapir provides comprehensive management for eyelid skin cancers. His expertise is widely recognized.
Dr. Steinsapir provides comprehensive management for eyelid skin cancers. His expertise is widely recognized.
The most common skin cancers of the eyelid are basal cell carcinoma and squamous cell carcinoma. These are usually caused by long-term sun exposure.
Dr. Steinsapir typically works with a Mohs’ cancer surgeon who performs the excision of the lesion using microscopic control. Dr. Steinsapir then does the reconstruction. This team approach provides the highest rate of cure and at the same time conserves the uninvolved eyelid by limiting the removal of normal tissue.
It is Dr. Steinsapir’s goal to provide the most natural reconstruction possible.
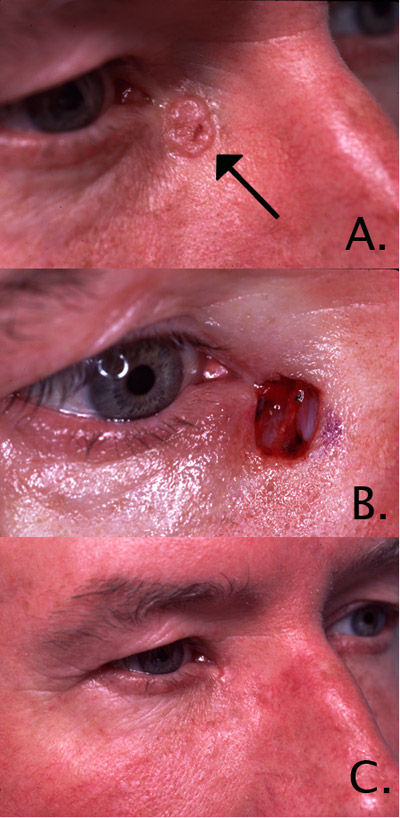
- Image A: The arrow points to the raised skin lesion with abnormal vascularity, raised pearly edges, and an area of ulceration that chronically bleeds. A biopsy by Dr. Steinsapir revealed it to be a basal cell carcinoma.
- Image B: A Mohs’ cancer surgeon, who works with Dr. Steinsapir, carefully removed the lesion. This method preserves the maximum of normal tissue and has the highest cure rate of the various treatment options.
- Image C: Dr. Steinsapir repaired the defect. Notice that the area has healed beautifully. One can’t tell that a large skin cancer had been present in the area.
Procedure: Midface Reconstruction
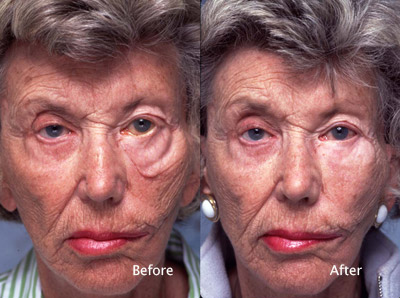
Cosmetic Concern:
74-year-old with long standing left facial paralysis following the removal of an acoustic neuroma from the brain stem.
Diagnosis:
- 1Left facial paralysis.
- Marked left lower eyelid atrophy.
- Left lower eyelid vertical inadequacy.
Treatment:
- Custom ePTFE left orbital rim implant.
- Left midface lift.
- Alloderm implant to the left lower eyelid.
Procedure: Repair of Prior Eyelid Surgery
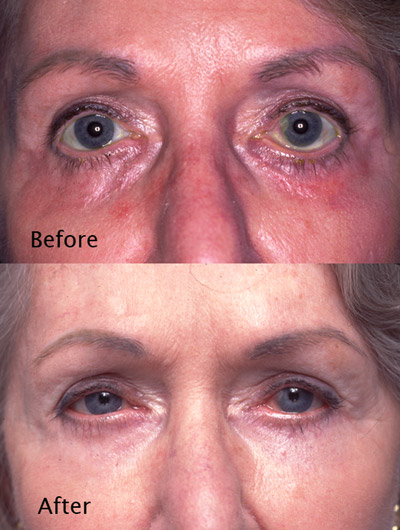
Cosmetic Concern:
64-year-old woman with a history of prior eyelid surgery. She was concerned about the pulled down lower eyelids. This was a direct result of her prior eyelid surgery. The muscle of the lower eyelids was damaged by that surgery and she has chronic dry eye symptoms as a result.
Diagnosis:
The lower eyelids had aggressive surgery that damaged both their appearance and function
Treatment:
The patient’s lower eyelids were reconstructed using graft material obtained from the roof of her mouth. This material was place behind the lower eyelid and avoided the necessity of a skin graft to the outside of the eyelid, which are difficult to conceal. To facilitate her repair, the cheek was also modestly lifted onto an ePTFE implant at the orbital rim. Due to the complexity of this repair, the right and left sides were repaired at separate surgeries that were 1 week apart.
Procedure: Upper Face Restoration
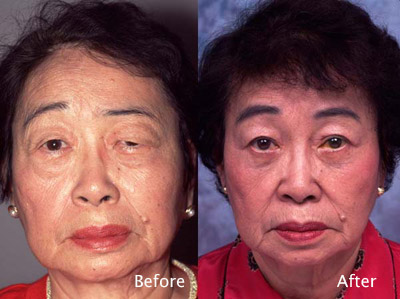
Cosmetic Concern:
74-year-old woman with left facial weakness following Bell’s palsy.
Diagnosis:
- Bell’s palsy
- Left forehead paralysis
- Pseudoherniated orbtial fat
Treatment:
- Endoscopic forehead lift
- Upper eyelid surgery
- Lower eyelid surgery
Procedure: Orbital & Midface Reconstruction
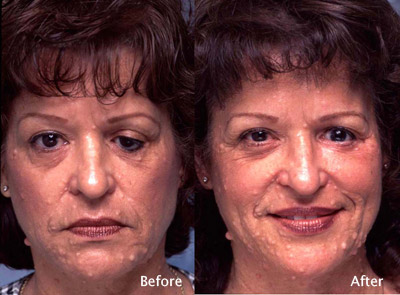
Cosmetic Concern:
This 51-year-old woman lost her left eye from a childhood orbital tumor. She consulted Dr. Steinsapir because her glass eye would not stay behind the left eyelids.
Diagnosis:
- Failure to retain ocular prosthesis.
- Inadequate orbital volume.
- Loss of inferior conjunctival cul-de-sac.
- Left upper eyelid ptosis.
Treatment:
- Replacement of left intraconal implant.
- Left midface surgery with ePTFE custom implant.
- Left lower eyelid reconstruction with hard palate graft.
Discussion:
Staged surgery was performed to rehabilitate her left orbit and midface. Many individuals who have lost an eye did not receive sufficient orbital volume at the time of their initial reconstruction. Addressing this issue can make a significant difference to the final result.
Procedure: Reconstructive Surgery
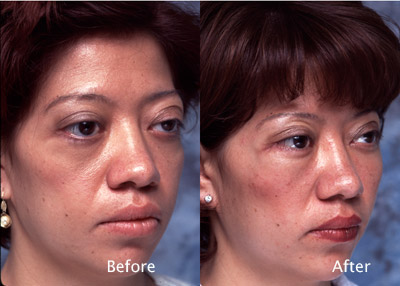
Cosmetic Concern:
This 28-year-old has a history of childhood thyroid eye disease. She had orbital decompression at the Jules Stein Eye Institute as well as several other eyelid procedures. However, she has difficulty closing the eyelids.
Diagnosis:
The patient had a profound benefit from her prior orbital surgery. However, she manifests poor projection of the inferior orbital rim. Consequently there is poor support for the lower eyelid and cheek. The lower eyelids hang below the curvature of the eyes. This prevents the eyelids from meeting upon lid closure.
Treatment:
The inferior orbital rim needs to be built up to support the cheek, which is vertically lifted onto the implant used along the orbital rim (Figure 2).
Procedure: Restorative Surgery
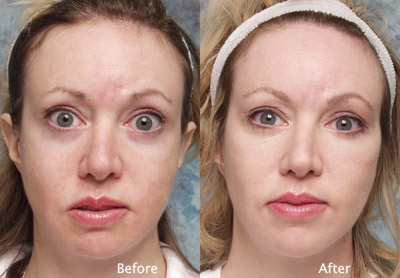
Cosmetic Concern:
34-year-old woman with a history of craniofacial surgery for maxillary hypoplasia. To address remaining aesthetic concerns she also had eyelid surgery and several face lifts. However, she feels that she still lacks the needed projection in her cheek-bones that would be best for her face.
Diagnosis:
- Glabellar scar secondary to flap perforation during forehead surgery.
- Bilateral upper eyelid retraction.
- Maxillary hypoplasia with deficient inferior orbital rim. Projection.
- Marked facial asymmetry.
Treatment:
- Augmentation of the orbital rims with custom hand carved orbital rim implant made from ePTFE.
- Vertical midface lift.
- Bilateral lateral canthoplasty
Discussion:
The patient needed additional volume in the midface. The ePTFE rim implant is custom carved for her particular anatomic deficit.
Procedure: Dermoid Reconstruction
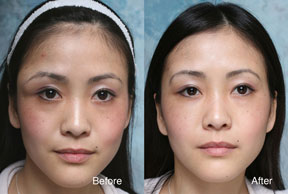
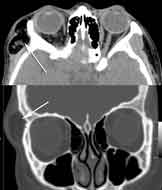
Cosmetic Concern:
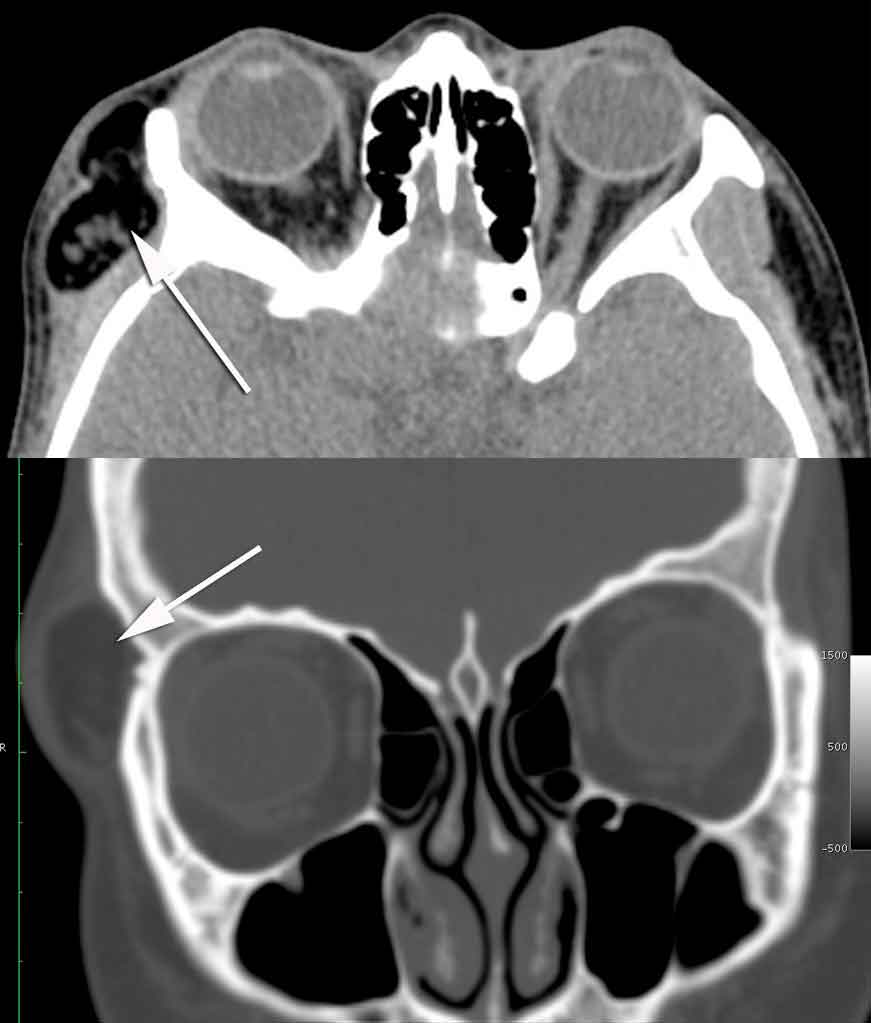
26-year-old woman with a life long history of a slowly expanding right orbital rim mass. She had seen physicians in the past and was advised that it was fat and that surgery was unnecessary. Dr. Steinsapir ordered a CT scan to assess the lesion. The arrows on the two CT images point to the lesion.
Diagnosis:
- Right orbital rim dermoid
Treatment:
Trans-temporal endoscopic dermoid removal. The standard approach for removing this type of dermoid is through an upper eyelid incision. However, scaring created by surgery can cause the upper eyelid fold to be affected. This was an important concern for a 26 year old. Dr. Steinsapir under took a much more technically difficult removal of the lesion through an endoscopic approach. Click here for the video of the surgery.