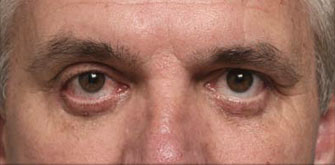
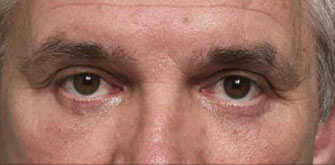
How to Fix Botched Lower Eyelids
The most frequent cause for an issue after lower eyelid surgery is not the shape of your cheekbone nor a negative vector eyelid. It is not that you failed to massage your lower eyelid as instructed by your surgeon. No, the number one cause for the fact that you have a lower eyelid problem after healing from your surgery is the choice of surgery by your cosmetic eyelid surgeon. It does not make your plastic surgeon a bad person unless they have made you feel responsible for lower eyelids gone wrong. The most common cause for an unsatisfactory outcome after lower eyelid surgery is the choice to perform the surgery through an incision on the outside of the eyelid.
Why did your plastic surgeon take this approach? The simplest answer is that it is customary for them because they were trained this way. It is what they were taught and the field persists in using this surgical approach because the alternative requires the surgeon to work very close to the eye. Different surgical specialties offer eyelid surgery. Many eyelid surgeons who perform surgery are not trained to work close to the eye. For that reason, they prefer to make their lower blepharoplasty through a skin incision. In the opinion of Dr. Steinsapir, that is generally a bad choice because many of the most common complications (such as botched lower eyelids) after lower eyelid surgery could have been avoided by using the transconjunctival approach rather than a transcutaneous approach.
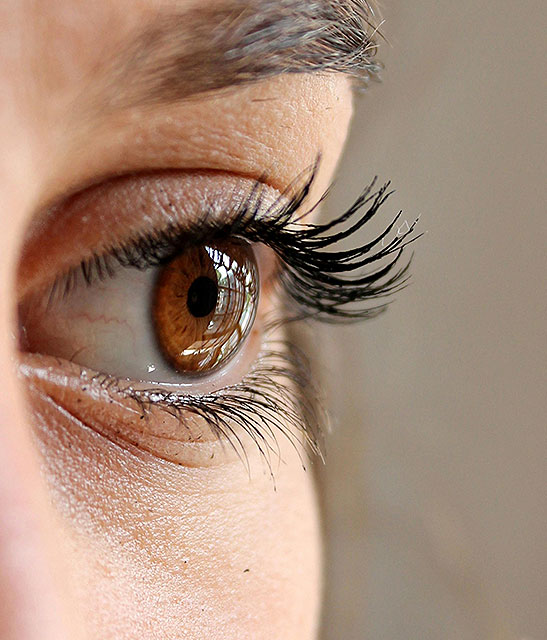
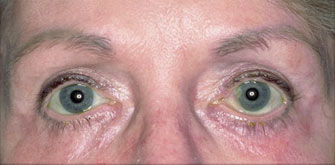
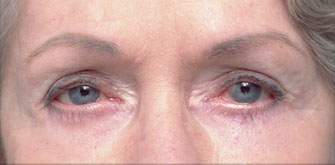
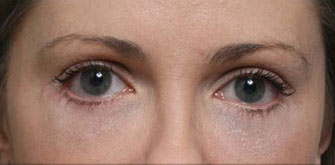
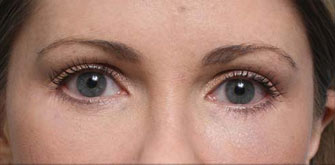
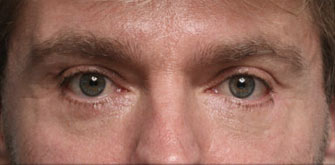
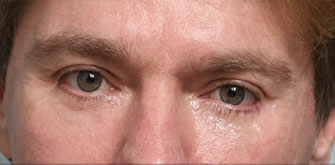
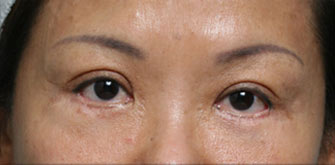
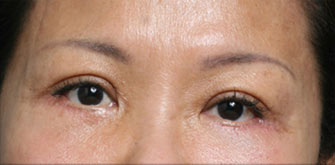
Under eye bags
The issues that bring most to consider surgery include a lower eyelid bag or dark circles caused by orbital fat that becomes visible in the lower eyelid, lower eyelid wrinkles, crows feet lines, and often a prominent muscle roll right at the edge of the eyelid. If you have had lower eyelid surgery and are reading this page because you had this type of eyelid surgery and now have a problem, it really does not matter why your eyelid surgeon chose this approach other than to understand they he or she thought they were making the right choice for you. Only it wasn’t. You are here reading this page because what you have been told so far doesn’t make sense.
Perhaps your relationship with your original eyelid surgeon has broken down. In most cases, the plastic surgeon who created the problem with their well-meaning surgery lacks the necessary skills to fix the problems they have created. They may even have tried to convince you that you have had a great result. For others, you may be coming to this site after one or more failed attempts to fixing lower eyelids gone wrong after your original surgical eyelid procedure.