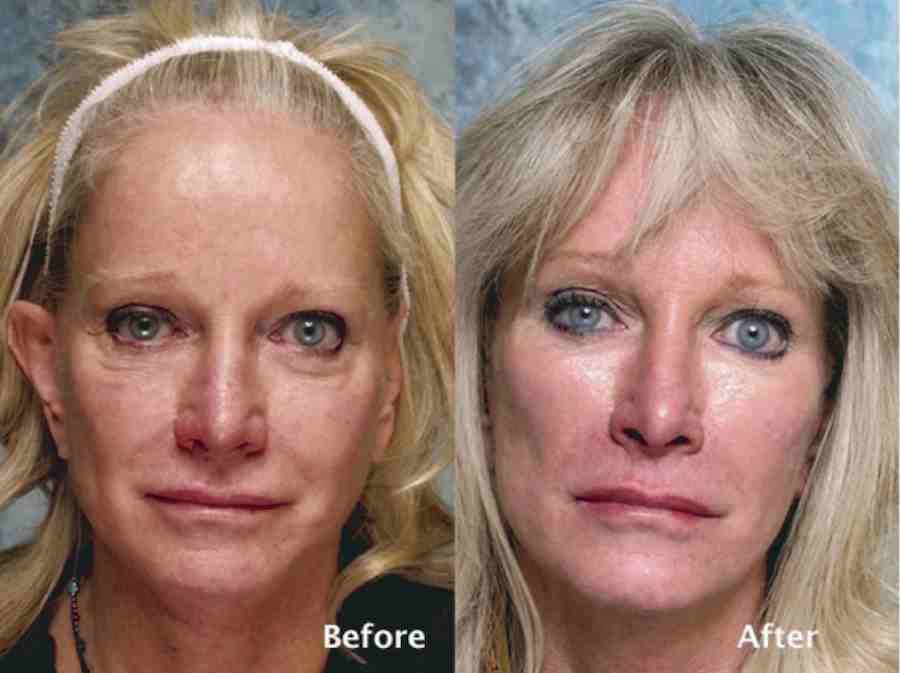
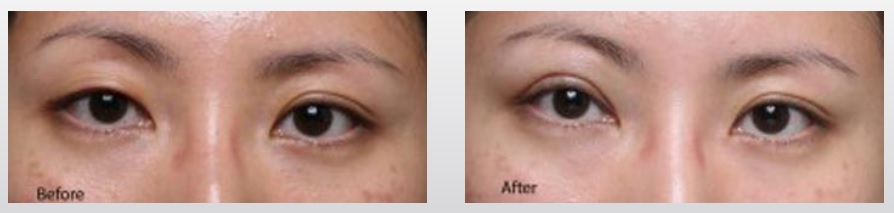
Potential immediate post-operative concerns include:
Dry Eye: the eyelids are like the windshield wipers of the eye, and post-surgical swelling of the eyelids can cause drying and irritation. This type of swelling can typically affect eye comfort for approximately ten days before swelling settles down enough for the eyelid to again move tears efficiently on the eye surface.
Motor Nerve Damage: Eyelid surgery cuts the small motor and sensory nerves to the eyelid. This can weaken the muscle that closes the eye (orbicularis oculi muscle), and the blink mechanism may be temporarily or permanently affected, causing long-term eye surface drying and dry eye symptoms (i.e. irritation, the sensation of burning, grittiness, redness). Fortunately, many of these closure issues resolve over time and can be treated with first-line approaches, such as artificial tears, bland ophthalmic ointment, plugging the tear drainage system, and/or taping the eyes closed. Should symptoms persist, surgery to improve eyelid closure may be required. In contrast to motor nerve damage, sensory nerve injuries are generally short-lived and are more likely to heal completely without additional surgery.
Hemorrhage: occurs as a result of blood vessels that are cut or damaged during the eye surgery, or from straining, coughing, or other activities following surgery that disrupt normal clot formation and may lead to the formation of large bruises. This bruising prolongs healing, and in more extreme cases, can disrupt the surgical result and even affect vision.
Retro-orbital hemorrhage: although some degree of post-operative bruising is normal, on rare occasions, a much more significant bruise can occur, potentially causing blindness. While these cases are very rare (about one in 300,000 cases), this concern is why you will be instructed to avoiding blood thinning medications and herbal products prior to surgery, and why Dr. Steinsapir may turn you down for surgery if you are required to be on a blood thinner after a heart valve replacement or recent stroke.
Superficial Bruising: although superficial bruising may not threaten the patient’s vision, severe bruises may cause swelling that can stretch a healing eyelid, potentially producing heaviness in the upper eyelid that requires surgical correction should it persist after 6 months. Similarly, in the lower eyelid, bruising stimulates the formation of extra collagen and scar tissue that can lead to permanent eyelid malposition, again necessitating reconstructive surgery.
Infection: infection after eyelid surgery is much less common than bruising. To reduce this risk further, antibiotics are often prescribed routinely after surgery to prevent this issue from arising. If an infection does develop after surgery, a change in the type of antibiotics may be warranted. Additional treatment options may include consultation with an infectious disease expert and intravenous antibiotics may rarely be necessary. Once the infection has cleared, if there is any loss of eyelid function or unanticipated scarring, this might warrant revision eyelid surgery to address these concerns. When reconstruction is needed in these circumstances, it is often reasonable to wait a full year before undergoing secondary surgery, as the tissue may eventually relax sufficiently enough to avoid revisional surgery.
Wound Dehiscence: This is the medical term to describe stitches that have come apart before the skin edges are healed together, causing the raw edges of the skin to separate and the wound to gape open. This unsightly complication commonly occurs in the upper eyelid, where the incision to remove excess skin is made. Although it is tempting to sew the raw edges back together immediately, there may be a low-grade infection causing the wound separation. For this reason, the best course of action is often simply to observe the area and keep it moist with extra antibiotic ointment. Perhaps the most surprising thing about wound dehiscence is how well it heals on its own. It has been Dr. Steinsapir’s experience that given time to fully heal, the body pulls the skin edges back together and no further intervention is required.
Chemosis: tissue swelling of the conjunctiva (the white of the eye). Mild chemosis will resolve on its own, while more severe chemosis requires aggressive lubrication with an ophthalmic ointment, occlusion with plastic wrap to prevent drying, and (if necessary) surgical intervention. Severe chemosis is very rare and is almost never seen with standard blepharoplasty—it is more commonly associated with procedures to tighten the lower eyelid (i.e. canthopexy and canthoplasty), more extensive midface procedures, or a pre-existing negative vector eyelid.
Double Vision: this rare complication is most often caused by the local anesthetic used to perform the surgery. In most cases, double vision resolves on its own within 1-2 hours; however, double vision that persists beyond the first day should be carefully measured and observed, as this may be a sign of injury to an adjacent eye muscle.
Scarring: scarring that may accompany post-surgical bruising typically improves over a period of months. In extremely rare cases, scars that do not ultimately heal in an acceptable fashion may benefit from revision eyelid surgery.