Chemical Peel Details Beverly Hills
Peel Procedure | Peel Case Studies
 The desire to rejuvenate the face and restore a youthful look is not unique to modern history. In the Edwin Smith Papyrus there is a description of an ointment that when applied was said to remove the signs of aging. The modern chemical peel dates from the nineteenth century. Ferdinand Hebra, a Viennese physician and a pioneer in dermatology was one of the first to describe the use of caustic agents on the face for the removal of lentigines or sun induced brown spots. The relationship between lay peelers and the progress of medical peelers is murky. Fifth Avenue “beautifiers” used phenol as early as the 1880s. This work was probably known to the physicians of the day. In the early 1960s, two groups of physicians filed and obtained patents for phenol solutions for chemical peeling. The technique of phenol peeling of the face became popularized with the work of Litton and Baker. It was the elegant and simple formula of Baker that was widely adopted by cosmetic surgeons. At the time that phenol peels were being broadly accepted in the medical community, Ayres described the use of various strengths of trichloroacetic acid. The 1980’s saw the evolution of chemical peeling with the enunciation of the concept of light, medium, and deep peels. The field has further matured with the introduction of alpha-hydroxy acid peels and role of retinoic acid.
The desire to rejuvenate the face and restore a youthful look is not unique to modern history. In the Edwin Smith Papyrus there is a description of an ointment that when applied was said to remove the signs of aging. The modern chemical peel dates from the nineteenth century. Ferdinand Hebra, a Viennese physician and a pioneer in dermatology was one of the first to describe the use of caustic agents on the face for the removal of lentigines or sun induced brown spots. The relationship between lay peelers and the progress of medical peelers is murky. Fifth Avenue “beautifiers” used phenol as early as the 1880s. This work was probably known to the physicians of the day. In the early 1960s, two groups of physicians filed and obtained patents for phenol solutions for chemical peeling. The technique of phenol peeling of the face became popularized with the work of Litton and Baker. It was the elegant and simple formula of Baker that was widely adopted by cosmetic surgeons. At the time that phenol peels were being broadly accepted in the medical community, Ayres described the use of various strengths of trichloroacetic acid. The 1980’s saw the evolution of chemical peeling with the enunciation of the concept of light, medium, and deep peels. The field has further matured with the introduction of alpha-hydroxy acid peels and role of retinoic acid.
>> Damaged Skin
>> Skin Care
>> Treatment Program
Agents for Chemical Peeling
>> Alpha Hydroxy Agents
>> Jessner’s Solution
>> Trichloroacetic Acid
>> Phenol
Chemical Peel Complications and Management
Like all procedures, the possibility of unwanted complications exist. The more commonly encountered issues are discussed here and are also discussed in detail as part of your consultation to help you make an informed choice.
>> Infection
>> Scarring
>> Ectropion and Lid Retraction
>> Color and Pigmentary Change
>> Allergic and Irritant Reactions
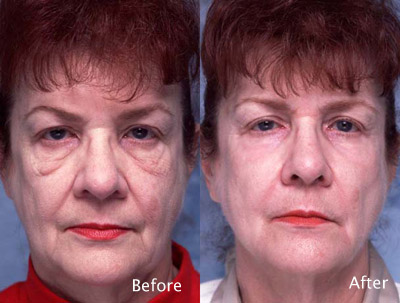
Peel Case Study
Frequently Asked Questions
Damaged Skin
The issues that affect your skin determine the type of peel procedures that will provide the most benefit. Common concerns include: acne with or without scaring, dark spots that have developed over time, skin aging from sun exposure, and intrinsic skin aging. It is important to understand that chronic sun exposure accounts for many of the changes associated with aged skin including fine lines, creases and deep furrows; loss of skin elasticity; scaly dry skin with irregular brown spots as well as premalignant or frankly malignant lesions; and an overall yellowish hue to the skin due to chronic sun damage.
If one were to look at the skin under a microscope, the outer layer of the skin called the epidermis demonstrates loss of organization called polarity. Polarity is the normal uniform maturation of the epithelium from the basal layer to the stratum corneum, the last layers of the skin. Individual cells may be atypical and these abnormalities can be seen in all the layers of the epithelium. The interface where the epithelium meets the upper level of the dermis flattens and the dermal matrix becomes disorganized. With sufficient sun damage, there is loss of the elastin. The ultimate result is a sagging skin that does not snap back to its original form when stretched. There is also loss of collagen.
Skin Care
The simplest of skin care programs consist of avoiding sun damage. Lifestyle changes include sensible sun avoidance, the use of sunscreens, and the use of either tretinoin (Retin A) or a low strength alpha hyrdoxy acid. Yes, this means selling the convertible and canceling the subscription for the tanning salon. If you have a history of seasonal affective disorder and are using the tanning for self-treatment, it is strongly advised that you seek professional help and find alternatives that are less harmful for your skin.
Photodamage accounts for about 90% of the changes we associate with aged skin. The bulk of this damage is from overexposure to ultraviolet (UV) light. The sun is the primary source of this exposure but artificial tanning lights are also intense sources of UV light, which are harmful to the skin. UV light includes wavelengths of light between 200 to 400nm. Skin is primarily affected by UVA (320-400nm) and UVB (290-320nm). Structures that absorb light in the skin are referred to as chromophores. In the UVB range, the light energy is absorbed by DNA. In the UVA range, proteins and lipids absorb the light. In the skin, melanin absorbs both UVA and UVB light. The concentration of melanin in the skin is a major factor in limiting UVB induced responses. UVA light penetrates deeper into the skin and causes elastotic degeneration deeper in the dermis than UVB light alone. As a consequence of this degeneration, photoaged skin is thicker than chronologically aged skin. These changes are more evident in fair skin individuals (skin types I-III) compared to dark skin individuals (skin types IV-VI).
Treatment Program
Sunscreens: Sunscreens work by absorbing, reflecting, and scattering UV light. The effectiveness of the sunscreen is indicated by a sun protection factor (SPF), which represents the ratio of the amount of radiation needed to produce redness with sunscreen to the amount of radiation needed to cause the same redness without the screen. There are now a number of commercially available sun blocks that contain tert-butylmethoxydibenzoylmethane which is effective at blocking UVA. Check the label of your sunscreen to be sure it covers both UVA and UVB. It has been estimated that regular sunscreen use during childhood and adolescence would decrease the lifetime incidence of nonmelanoma skin cancers by about 80%.
Tretinoin: In 1972, topical tretinoin (Retin A, Ortho) received FDA approval for the treatment of acne. However, in 1988 a placebo-controlled study demonstrated the value of tretinoin in improving the appearance of photoaged skin. Subsequent studies continue to support the value of tretinoin in both photoaged and chronologically aged skin. Finally, in 1996, the FDA also approved the use of tretinoin for the improvement of fine wrinkles making this one of the few products the FDA has approved for wrinkle reduction. Tretinoin also appears to prevent the development of squamous cell carcinomas in actinically damaged skin. The exact mechanism of tretinoin is not known. Retin A is available in several strengths and forms. We favor the use of Retin A cream 0.05% every fifth night until the skin adjusts to the product.
Alpha Hydroxy Agents
Alpha Hydroxy acids (AHA) are derived from fruit and dairy products. Glycolic acid is the most commonly used agent in this category. Glycolic acid like other AHA produces a smoother skin. When these products are combined with skin bleachers, there is a synergistic effect that facilitates the lightening of the skin. With chronic use of glycolic acid, new collagen and elastin are seen in the dermis. Glycolic acid also appears to help in the treatment of acne vulgaris. This may be related to the desquamation of keratinous plugs, which are central to the formation of new pimples.
Glycolic acid products are available in a variety of strengths and formulations. Lower concentration products (2-15%) are available as over-the -counter skin rejuvenation products. Higher strengths (8-30%) are distributed to estheticians for freshening facials and the 40-70% agents are available to the cosmetic surgeon for mild peeling. Stronger glycolic acid is effective at treating mild brown spots, melasma and skin darkening associated with long-term perfume use. The strength of a glycolic acid peel is dependent on it’s concentration, pH, and the length of time the acid acts on the skin before it is neutralized. Typically, a series of peels are performed to achieve a desired result. Stronger, in office peels can be combined with the use of mild at home products to create a very effective skin care program.
Jessner’s Solution
Jessner’s solution is a combination of resorcinol, salicylic acid, and lactic acid. It is a mild peeling agent. It can be combined with Trichloroacetic acid (TCA) 35% to enhance the penetration of the TCA. TCA 35% is a mild to moderate peeling agent. However, it penetrates more deeply into the papillary dermis following the application of Jessner’s solution creating a peel of moderate depth with a good safety margin.
Trichloroacetic Acid
Trichloroacetic acid (TCA) is used in a variety of strengths depending on the desired effect. Mild freshening peels can be obtained with a TCA 10% solution. This agent produces a mild burn and minimal frosting. The patient experiences redness and mild desquamation to reveal a fresher, smoother skin. This effect can be enhanced up to 20%. At concentrations of 25 to 35%, the peel is sufficiently uncomfortable that patients benefit from regional anesthesia and oral or intravenous sedation. Trichloroacetic acid solutions in concentrations above 50% are unpredictable and can result in unexpected scaring. In the 35% concentration, patients will experience a frosting of the skin following the application. Over 24 hours the skin initially reddens and then darkens. At 48 to 72 hours following the peel, the skin begins to shed to reveal a pink fresh epithelium that may take several days before it is completely intact. Post-operative skin care can be managed with gentle wound debridement and bland petrolatum dressing until the epithelium is intact. There is little tendency for hypopigmentation and no systemic toxicity.
Phenol
Phenol and Baker’s formula are powerful and highly effective agents for chemical peeling of the face. Phenol 89% solution is considered a medium deep peeling agent and is effective at addressing all but the deepest lines. Both phenol and Baker’s phenol are capable, when used properly, of producing an over all tightening effect on the skin of the face that can, in select patients, rival the results of a face lift. Both agents are able to significantly improve sun damage, sun-spots, actinic keratosis and frank in-situ squamous cell carcinomas. Baker’s solution is capable of penetrating deep to the reticular dermis and effect a greater degree of change. When studied with a microscope, phenol causes tissue injury to the epithelium with varying degrees of edema and inflammation in the reticular dermis. The result is regeneration of the epithelium from skin appendages like hair follicles and sweat glands resulting in dermal thickening, new collagen, and elastin deposition. The relative strength of these agents necessitates caution in their application. Over doing it can result in facial scaring. Dr. Steinsapir believes that it is better to be conservative and avoid this type of problem. Full-face phenol applications are associated with cardiac arrhythmia. Fortunately almost all patients do not need full-face phenol applications. By limiting the application of phenol to only small areas of the face that need the greatest help, cardiac irritation is avoided. By minimizing the use of phenol, the discomfort associated with its indiscriminate use is entirely avoided. This makes it possible to have a full-face peel with profound results under local anesthesia with a minimal dose of pain medication. Patients who have had a phenol peel can take up to 10 to 12 days to heal. During this period, the skin is gently debrided with frequent showers and dressed with a bland petrolatum. The skin can stay red up to 4-6 months often necessitating cover up with make up for some. Men often find that this slight redness blends easily into their complexion and does not raise questions about what they have had done.
Infection
Bacterial: Bacterial infection following a chemical peel is rare. The use of prophylactic antibiotics following a chemical peel is Dr. Steinsapir’s routine. An infection may occur anytime after the second post-operative day. The signs are prominent swelling of the lids, significant amounts of devitalized skin and redness. The mainstay of treatment is enhanced local wound care measures, antibiotic, daily examination by Dr. Steinsapir, and reinforcement of sound wound care measures. He has found that infections most often result from not closely following post-procedure instructions. The procedure represents an important investment in time, energy, and expense and it is essential to follow Dr. Steinsapir’s advice.
Herpes viral infections are primarily associated with medium or deep chemical peels. There is almost always a history of prior infection. The diagnosis of a herpetic infection may be difficult to make. Complaints of pain and malaise are suggestive of herpes but are not always present. A fever is often associated with an outbreak. Wounded skin that was healing well and then regressed is suggestive of a herpetic infection. Valtrex® has been very helpful in preventing these sores and therefore it is routinely part of the care following a peel.
Scarring
Scarring may occur after chemical peeling. Fortunately, scarring and unfavorable textural changes are uncommon. Certain areas of the face are prone to slow healing and scarring: the inner aspect of the lower eyelid and along the jaw line. These areas possess thin skin and in the case of the inner lower eyelid a relatively low density of adnexal skin structures. Potential early scarring usually will present as persistent redness. In such cases, frequent massage of the involved skin can be effective to reduce skin stiffness. In time, the redness will fade, and skin thickening will decrease with flattening and softening of the area. Dr. Steinsapir follows his patients closely after a chemical peel specifically to avoid these types of issues. If necessary, the skin may be treated with Kenalog, 5-flurouracil or even topical steroid cream to reduce the likelihood of a scar development. Intralesional or topical corticosteroid use can cause skin atrophy and the development of telangiectasias, which after the fact can be treated with IPL. Mild scarring usually fades during a period of 3 to 12 months. With appropriate management mild scarring typically leaves at worst a slight textural change that is generally barely noticeable.
Ectropion and Lid Retraction
A transient lower eyelid malposition is common in cases of medium to heavy peeling in older patients with lower eyelid laxity. This minor out-turning of the lid margin and slight pulling down of the lower eyelid typically resolves when the skin relaxes after the contraction phase of wound healing. This can result in transient corneal exposure. When this is the case, there can be a foreign body sensation in the eyes. Nightly use of a bland ophthalmic ointment and use of an artificial tear preparation during the day until the anatomic problems are improved usually addresses these symptoms. In patients who are undergoing simultaneous eyelid surgery, a lateral canthal resuspension may be considered to reduce the possible occurrence of eyelid malposition.
Color and Pigmentary Change
Permanent hypopigmentation is an expected and common result following peeling with stronger agents such as TCA 50%, phenol 89%, and Baker’s phenol mixture. Splotchy hyperpigmentation is also a common occurrence early after re-epithelialization in dark-skinned patients. It usually is not permanent and is treated with strict sun avoidance, tretinoin cream 0.05% or 0.1% cream applied at bedtime, and 4% to 6 % hydroquinone cream applied in the morning. In almost all cases, one to three months of this treatment will resolve the problem.
Redness always occurs to some degree following peeling, and is proportional in its intensity and duration to the depth of the peel in that particular individual. The redness following TCA 35% persists for between two weeks to four weeks; following phenol 89% redness may persists for 3 to 6 months, and following a Baker’s phenol for 5 to 12 months. The redness can be camouflaged successfully with makeup until it resolves.
Allergic and Irritant Reactions
Polysporin and bacitracin topical antibiotic preparations should be avoided because they can cause an allergic reaction. For this reason, bland petrolatum such as Vaseline® is recommended to keep the peeled skin from drying out.
Why do people choose to have a chemical peel? These treatments can be precisely tailored for the individual. By carefully selecting the agents for the peel, it is possible to perform these amazing treatments in an office setting with minimal medications. While there is down time and after care, the results benefit the entire face and the results are remarkably natural. Is a chemical peel right for you? Your personal consultation with Dr. Steinsapir will answer that question.
I am getting a monthly Jessner’s peel by my aesthetician. How does that differ from the peels that Dr. Steinsapir performs?
The Jessner’s peel is a very mild peel. Even the low concentration trichloroacetic acid peels such as the 10 and 15% concentration reach deeper into the skin. It is likely that a 15% TCA peel performed two or three times a year would produce the same results or even more dramatic results than you currently achieve with the Jessner’s peel that you find necessary to repeat on a monthly basis.
My cosmetic surgeon tells me that chemical peels are obsolete and has recommended that I get a series of Fraxel® laser treatments instead. What does Dr. Steinsapir think of Fraxel®?
Fraxel® is fractional CO2 laser resurfacing. In general, these are relatively mild treatments designed to be well tolerated and with no down time. Because they are mild, the degree of improvement is limited. It will freshen the complexion but does not create a lot of tightening. The equivalent treatment with a chemical peel might be a 20% TCA peel of the face. The good news is that you are unlikely to be harmed by this type of treatment but you may also not feel that you got your monies worth depending on what you were charged. In defense of the fees charged for Fraxel®, the device is very expensive and this is reflected in what is charged for the service. By the way, peels are not obsolete, it is just that very few surgeons are trained to perform chemical peels like Dr. Steinsapir.
My cosmetic surgeon has recommended that I have CO2 laser resurfacing. I am a little nervous about the treatment especially after reading in his brochure that it is normal to have a result that leaves the face lighter than the neck. Is a chemical peel an alternative to CO2 laser resurfacing?
Dr. Steinsapir believes that CO2 laser resurfacing is a failed technology. It offered a lot of promise when it was first introduced. It is possible to have a good results with CO2 laser but only if the treatment is performed on a person with the right complexion. In general, the thermal injury created by CO2 laser injures the melanocytes of the skin and results in hypopigmentation. There are also often textural abnormalities in the skin after a CO2 laser treatment. The solution is avoiding the CO2 laser and having a customized full-face chemical peel. Call the office to schedule a personal consultation with Dr. Steinsapir and learn if a chemical peel is right for you.
I am thinking of having a laser peel. What are these and what are the alternatives?
Generally, a laser peel is performed with an erbium laser, which is used in a single pass. This ablates off only a few layers of skin and is usually comfortable with a topical numbing cream. However, the treatment is very superficial and therefore the results are very mild. How mild? The treatment can be equivalent to a microdermabrasion, which is very mild indeed. Therefore the service should be very inexpensive or it will not be worth the price paid.
Several years ago, I had laser resurfacing of my lower eyelids. I developed hyperpigmentation of the skin. The doctor who treated me said that this was normal and would resolve in time but never did. Is there anything that can be done for this issue?
A consultation with Dr. Steinsapir will prove to be very helpful in fully answering this question. However, in general, there are a number of treatments for post-laser hyperpigmenation. Dr. Steinsapir has successfully treated this condition with both fotofacial® and chemical peels. So we encourage you to come in for a personal consultation to learn what can be done.
I have heard that chemical peels are very uncomfortable. How will I know if I can tolerate a chemical peel?
The key with having a comfortable chemical peel is in preparation. Dr. Steinsapir has evolved an entire system for making a comfortable full-face chemical peel. The result is an incredibly effective treatment that is surprisingly comfortable. You might be shocked to learn that most of our patients find they only need extra-strength Tylenol® after their chemical peel.
Return to Chemical Peel
 The desire to rejuvenate the face and restore a youthful look is not unique to modern history. In the Edwin Smith Papyrus there is a description of an ointment that when applied was said to remove the signs of aging. The modern chemical peel dates from the nineteenth century. Ferdinand Hebra, a Viennese physician and a pioneer in dermatology was one of the first to describe the use of caustic agents on the face for the removal of lentigines or sun induced brown spots. The relationship between lay peelers and the progress of medical peelers is murky. Fifth Avenue “beautifiers” used phenol as early as the 1880s. This work was probably known to the physicians of the day. In the early 1960s, two groups of physicians filed and obtained patents for phenol solutions for chemical peeling. The technique of phenol peeling of the face became popularized with the work of Litton and Baker. It was the elegant and simple formula of Baker that was widely adopted by cosmetic surgeons. At the time that phenol peels were being broadly accepted in the medical community, Ayres described the use of various strengths of trichloroacetic acid. The 1980’s saw the evolution of chemical peeling with the enunciation of the concept of light, medium, and deep peels. The field has further matured with the introduction of alpha-hydroxy acid peels and role of retinoic acid.
The desire to rejuvenate the face and restore a youthful look is not unique to modern history. In the Edwin Smith Papyrus there is a description of an ointment that when applied was said to remove the signs of aging. The modern chemical peel dates from the nineteenth century. Ferdinand Hebra, a Viennese physician and a pioneer in dermatology was one of the first to describe the use of caustic agents on the face for the removal of lentigines or sun induced brown spots. The relationship between lay peelers and the progress of medical peelers is murky. Fifth Avenue “beautifiers” used phenol as early as the 1880s. This work was probably known to the physicians of the day. In the early 1960s, two groups of physicians filed and obtained patents for phenol solutions for chemical peeling. The technique of phenol peeling of the face became popularized with the work of Litton and Baker. It was the elegant and simple formula of Baker that was widely adopted by cosmetic surgeons. At the time that phenol peels were being broadly accepted in the medical community, Ayres described the use of various strengths of trichloroacetic acid. The 1980’s saw the evolution of chemical peeling with the enunciation of the concept of light, medium, and deep peels. The field has further matured with the introduction of alpha-hydroxy acid peels and role of retinoic acid.
